Essential Infection Control Tools for Every Healthcare Facility
Infection control remains one of the most important priorities in any healthcare setting. From large hospitals to small clinics and day procedure centres, preventing the spread of harmful microorganisms is essential for patient safety and staff protection. Strong infection control practices also help reduce complications, shorten recovery times, and maintain public confidence in healthcare services.
Behind every safe clinical environment is a structured system supported by reliable equipment. The right tools help ensure that cleaning, sterilisation and contamination prevention are carried out consistently and effectively. As healthcare demand grows across Australia, so does the need for dependable infection control systems supported by modern equipment and clear procedures.
Why Infection Control Tools Matter in Healthcare Settings
Healthcare environments naturally involve exposure to bacteria, viruses, and other pathogens. Without proper controls, these can spread quickly between patients, staff, and equipment surfaces.
Effective infection control reduces hospital-acquired infections, protects vulnerable patients, and supports compliance with national safety standards. It also reduces operational costs by preventing outbreaks that can disrupt services.
Facilities that invest in proper systems and equipment create safer conditions for everyone involved in patient care.
The Role of Equipment Quality in Infection Prevention
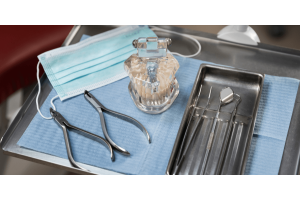
Not all infection control tools perform equally. Quality and compliance play a major role in effectiveness. High-grade stainless steel instruments are easier to clean and sterilise. Durable PPE materials reduce the risk of tears or failures during use. Reliable disinfectant systems ensure consistent performance across repeated cycles. Poor-quality equipment can compromise infection control efforts, even when protocols are followed correctly. This is why procurement decisions are so important for healthcare facilities.
Core Categories of Infection Control Equipment
Infection prevention relies on multiple layers of protection. Each category of equipment plays a specific role in maintaining hygiene and reducing contamination risks.
· Cleaning and Surface Management Tools
Daily cleaning is the foundation of infection control. Microfibre cloths, disinfectant wipes, mop systems, and surface sprays are essential healthcare hygiene tools used across all clinical areas.
High-touch surfaces such as bed rails, door handles, and treatment chairs require frequent cleaning. Using hospital-grade disinfectants ensures pathogens are effectively reduced. Colour-coded cleaning systems are also common in Australian facilities to prevent cross-contamination between zones.
· Sterilisation Systems
Instrument sterilisation is critical in preventing infection during procedures. Autoclaves, ultrasonic cleaners, and drying cabinets are widely used to ensure instruments are free from microbial contamination.
These medical sterilisation instruments operate using heat, pressure or chemical processes to achieve high-level disinfection. Proper loading, cycle monitoring, and maintenance are essential to ensure effectiveness. Reusable surgical tools must always pass through validated sterilisation cycles before reuse. This helps maintain patient safety and supports compliance with national guidelines.
· Personal Protective Equipment
Personal protective equipment, commonly known as PPE, forms a barrier between healthcare workers and infectious agents. Gloves, masks, gowns, and eye protection are standard components in most clinical environments.
PPE use is particularly important during procedures that involve bodily fluids or respiratory exposure. Correct donning and doffing procedures are equally important to prevent accidental contamination.
Compliance and Regulatory Standards in Australia
Australian healthcare facilities must follow strict infection control guidelines set by national authorities. These standards outline cleaning procedures, sterilisation requirements, and equipment expectations.
Regular audits and inspections ensure compliance is maintained. Facilities that fail to meet standards may face operational risks and reputational damage. Working with trusted suppliers of surgical equipment helps facilities maintain consistent quality and regulatory compliance across all infection control systems.
Disinfection and Waste Management Systems
Beyond tools used directly on patients, infection control also depends on how waste and contaminated materials are handled.
· Disinfection Protocols
Alcohol based solutions, chlorine-based disinfectants, and hydrogen peroxide systems are widely used in clinical environments. Each solution is selected based on surface type and risk level.
Regular disinfection schedules help maintain consistency and reduce the risk of missed areas. Staff training plays a key role in ensuring these protocols are followed correctly.
· Clinical Waste Disposal
Safe disposal of sharps, contaminated materials, and biological waste is essential. Colour-coded bins and sealed containers help separate infectious waste from general waste streams. Incorrect disposal can increase infection risk and create environmental hazards. Clear procedures and staff awareness are necessary for safe waste handling.
Facilities often work closely with MediTools Pty Ltd, a reliable medical equipment supplier in Australia, to ensure compliance with disposal regulations and to maintain reliable access to approved products.
Instrument Reprocessing and Workflow Safety
Instrument reprocessing is one of the most critical parts of infection control. It ensures that reusable equipment is safe for the next patient.
· Cleaning, Inspection, and Packaging
Before sterilisation, instruments must be carefully cleaned to remove visible debris. Manual cleaning and automated washers are both used, depending on facility size and workload. After cleaning, instruments are inspected for damage or residue. Proper packaging ensures sterility is maintained until the point of use.
· Tracking and Traceability
Many facilities now use digital tracking systems to monitor instrument usage and sterilisation cycles. This helps identify any issues quickly and ensures accountability across departments. Traceability is especially important in high-turnover environments such as surgical units and emergency departments.
Training and Staff Awareness
Even the best equipment is only effective when used correctly. Staff training is a core part of infection control programs.
· Correct Usage Practices
Healthcare workers must understand how to use PPE, operate sterilisation equipment and follow cleaning schedules. Small mistakes can lead to contamination risks.
Regular refresher training helps maintain awareness and ensures staff stay updated with current guidelines.
· Building a Safety Culture
Infection control works best when it is part of everyday practice rather than a checklist task. Encouraging accountability and open communication helps create a safer clinical environment.
Technology in Modern Infection Control
Technology continues to improve how infection prevention is managed in healthcare settings. Automated cleaning systems reduce human error and improve consistency. Digital monitoring tools track sterilisation cycles and provide real-time data. UV disinfection systems are also being introduced in some facilities for additional surface cleaning support. These advancements help reduce manual workload while improving accuracy and safety outcomes.
Challenges in Infection Control Management
Despite strong systems, infection control remains challenging. High patient turnover, staffing pressures, and resource limitations can impact consistency.
Maintaining equipment, updating protocols, and ensuring ongoing training all require time and investment. However, these efforts are essential to prevent larger issues such as outbreaks or cross-contamination incidents.
Final Thoughts
Infection control is a fundamental part of safe healthcare delivery. Every facility relies on structured systems supported by reliable tools and consistent practices. From cleaning systems and sterilisation devices to protective equipment and waste management solutions, each component plays a role in reducing risk and protecting patients.
Strong infection prevention supplies combined with proper training and compliance help create safer healthcare environments across Australia. For facilities seeking dependable solutions, MediTools Pty Ltd provides high-quality surgical equipment in Australia that supports infection control standards.
Disclaimer
The content provided here on the sterilization, cleaning, and reprocessing of surgical and medical instruments is strictly for informational and educational purposes only. This information is not a substitute for professional training, certification, or the manufacturer's official Instructions for Use (IFU). Sterilization is a critical, complex process that demands strict adherence to regulatory standards; improper technique can cause serious harm, including patient infection. All healthcare personnel must follow their facility's established protocols and the specific IFU for every instrument and piece of equipment. By using this blog, you agree that the author/owner holds no liability for any damages or consequences resulting from the application or misuse of this information.