Minimally Invasive Surgery Tools: What Healthcare Professionals Should Know
Minimally invasive surgery has transformed operating theatres across Australia. Smaller incisions, shorter hospitalisations, and quicker recovery periods have become the norm in various medical specialties. From general surgery to gynaecology, urology, and orthopaedics, clinicians are increasingly relying on precise, reliable equipment to deliver safe outcomes.
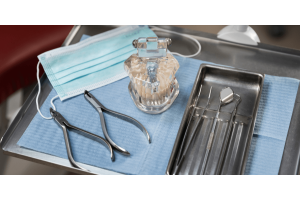
At the centre of this shift are minimally invasive surgery tools designed to support accuracy through limited access points. For healthcare professionals, understanding the design, handling, and maintenance of these instruments is essential for consistent performance and patient safety.
Why Minimally Invasive Surgery Continues to Grow
Australian hospitals have steadily expanded minimally invasive approaches over the past two decades. These techniques are associated with reduced postoperative pain, lower infection risk, and faster return to normal activity compared with traditional open procedures.
Shorter admissions also reduce pressure on hospital beds and support efficient use of resources. For regional and metropolitan facilities alike, these benefits are significant. As demand grows, surgical teams must stay informed about evolving equipment standards and best practices.
Core Categories of Instruments
Modern operating rooms rely on a coordinated system of devices rather than a single tool. Each category plays a distinct role during procedures.
Access and Visualisation Equipment
Access typically begins with trocars and cannulas that create stable entry points. Once ports are placed, visualisation becomes critical. High definition laparoscopes and camera systems provide magnified internal views, allowing surgeons to work with precision.
Insufflators maintain pneumoperitoneum in abdominal cases, ensuring adequate working space. Reliable imaging and stable pressure control are foundational elements of safe minimally invasive procedures.
Hand Instruments and Energy Devices
Fine control is achieved through specialised surgical instruments for minimally invasive procedures such as graspers, dissectors, scissors, and needle holders. Long shafts and ergonomic handles are designed for controlled movement within confined spaces.
Energy devices, including monopolar and bipolar instruments, ultrasonic shears, and advanced vessel sealing systems, assist with haemostasis and tissue division. Proper training in energy settings and insulation integrity is vital to prevent thermal injury.
Laparoscopic Sets
A comprehensive set of laparoscopic surgical instruments typically includes atraumatic graspers, clip appliers, suction irrigation systems, and specimen retrieval bags. Each component must function smoothly to avoid delays during surgery.
Australian facilities often standardise instrument trays to streamline workflow and reduce setup time. Consistency in layout supports theatre efficiency and minimises errors.
Design Considerations and Ergonomics
Minimally invasive surgery can be physically demanding for surgeons and theatre staff. Prolonged procedures require steady posture and controlled movements. Poorly designed instruments may contribute to fatigue or musculoskeletal strain.
Ergonomic handles, balanced weight distribution, and smooth articulation mechanisms improve comfort and reduce hand stress. Rotating shafts and angled tips enhance access to difficult anatomical areas.
Hospitals sourcing medical instruments in Australia from trusted sellers, like MediTools Pty Ltd, should consider both clinical performance and user comfort. Feedback from surgical teams is valuable when assessing new product lines.
Material Quality and Durability
High-quality stainless steel and advanced alloys remain standard in reusable instruments. These materials resist corrosion and withstand repeated sterilisation cycles. For certain components, polymer and composite materials reduce weight while maintaining strength.
Single-use instruments are increasingly common in some specialties. They eliminate reprocessing requirements but must meet strict safety and performance standards. Facilities must balance cost, sustainability, and infection control considerations when selecting between reusable and disposable options.
The rise of advanced surgical instruments incorporating articulating tips and integrated energy delivery systems has added further complexity. Regular inspection and adherence to manufacturer guidelines are essential to maintain functionality.
Sterilisation and Infection Control
Effective sterilisation is non-negotiable in any surgical setting. Minimally invasive instruments often feature narrow lumens and complex joints that require thorough cleaning.
Australian guidelines from the National Health and Medical Research Council outline best practices for infection prevention and control. Pre-cleaning at the point of use, ultrasonic cleaning, and validated sterilisation cycles help reduce contamination risk.
Instrument tracking systems are also becoming standard in many hospitals. These systems record usage, reprocessing history, and maintenance schedules, supporting traceability and compliance.
Training and Competency
Introducing new instruments requires structured education. Simulation-based training allows surgeons and theatre nurses to practise handling and coordination before using equipment in live cases.
Credentialing processes often include supervised procedures to ensure competency. Ongoing professional development is equally important as technology continues to advance.
Hospitals should also provide clear protocols for troubleshooting equipment issues during surgery. Familiarity with backup instruments and contingency plans reduces stress in high-pressure situations.
Technology Integration in Modern Theatres
Digital integration has become a defining feature of contemporary operating rooms. High definition imaging, three-dimensional visualisation, and robotic platforms are increasingly used alongside traditional laparoscopic systems.
Robotic-assisted surgery relies on specialised consoles and instrument arms controlled remotely by the surgeon. Although distinct from conventional laparoscopy, these systems share similar principles of minimal access and precision.
Integration with electronic medical records and imaging systems streamlines documentation and improves coordination among multidisciplinary teams.
Cost and Procurement Considerations
Budget constraints remain a reality across public and private sectors. Procurement teams must assess upfront costs alongside long-term value.
Reusable surgical instruments for minimally invasive procedures may require a higher initial investment but offer durability over time. Service agreements and warranty terms should be reviewed carefully.
Engaging with reputable suppliers of medical and surgical instruments ensures compliance with Therapeutic Goods Administration regulations. Transparent documentation, training support, and reliable after-sales service are critical factors in purchasing decisions.
Risk Management and Patient Safety
Although minimally invasive surgery offers many benefits, complications can still occur. Equipment failure, insulation defects, and poor visualisation are known risk factors.
Routine inspection of insulation integrity, especially in energy devices, reduces the likelihood of unintended burns. Clear communication between surgeons and theatre staff during instrument exchange also improves safety.
Checklists before and after procedures help confirm correct instrument counts and functionality. A culture of reporting and reviewing equipment-related incidents supports continuous improvement.
Final Thoughts
Minimally invasive surgery is firmly established in Australian healthcare. Safe and effective outcomes depend not only on surgical skill but also on the quality and reliability of minimally invasive surgery tools used in every procedure.
Healthcare professionals must remain informed about instrument design, sterilisation standards, ergonomic considerations, and emerging technologies. Careful selection, consistent maintenance, and structured training all contribute to strong clinical performance.
For hospitals and clinics seeking dependable solutions, MediTools Pty Ltd provides a comprehensive range of high-quality products and expert guidance. Connect with our team today to source trusted medical surgical instruments that support precision and patient safety in modern operating theatres.
Disclaimer
The content provided here on the sterilization, cleaning, and reprocessing of surgical and medical instruments is strictly for informational and educational purposes only. This information is not a substitute for professional training, certification, or the manufacturer's official Instructions for Use (IFU). Sterilization is a critical, complex process that demands strict adherence to regulatory standards; improper technique can cause serious harm, including patient infection. All healthcare personnel must follow their facility's established protocols and the specific IFU for every instrument and piece of equipment. By using this blog, you agree that the author/owner holds no liability for any damages or consequences resulting from the application or misuse of this information.